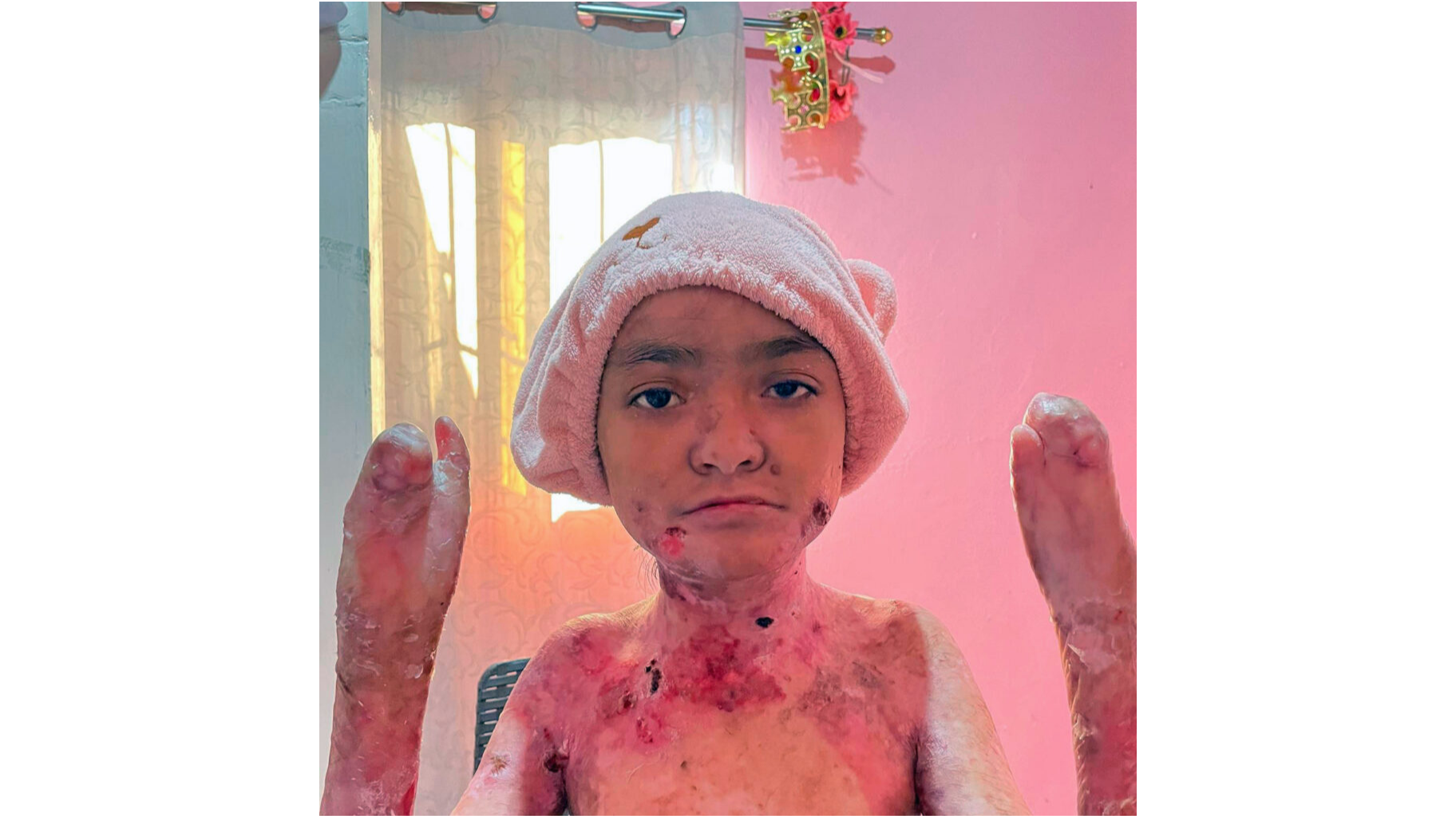
Key Takeaways
- A multimodal pain management approach combining medications, distraction techniques, and proper dressing selection significantly reduces suffering during wound care for children with Epidermolysis Bullosa (EB) and rare craniofacial cancers.
- Timing severe pain medicine approximately 30 to 60 minutes before dressing changes maximizes effectiveness for pediatric patients.
- Non-adherent silicone-based dressings and gentle warm water soaks are essential for minimizing the trauma of bandage removal.
- Specialized relief programs provide direct medical supplies to over 5,100 children worldwide, addressing the $160,000 annual medical burden that families in underserved regions often face.
- Virtual reality and behavioral distraction can reduce both physical pain and psychological trauma when paired with proper caregiver training.
For families managing the daily challenges of Epidermolysis Bullosa care, dressing changes represent one of the most dreaded yet necessary aspects of treatment. These routine procedures, required for preventing infection and promoting healing, can become traumatic experiences that leave both children and parents emotionally and physically exhausted.
Charities working to support children with EB emphasize that immediate medical relief is the priority. Every intervention should focus on the urgent need to stop excruciating pain, as these children cannot wait for long-term research promises.
Why Dressing Changes Cause Excruciating Pain for Children with EB
Epidermolysis Bullosa (EB) creates a relentless cycle of pain during wound care. This genetic condition causes the skin to be as fragile as a butterfly’s wing, often leading to up to 80% skin loss at any given time. The fragility causes the skin to blister and separate with minimal friction, leaving raw, exposed nerve endings that react intensely to touch, temperature changes, and bandage removal. Unlike typical wounds that develop protective scabs, EB lesions remain perpetually sensitive, making even the most gentle handling a source of significant distress.
The frequency of dressing changes compounds this suffering. Children with severe EB may require daily or twice-daily wound care sessions that can last up to four hours. This repetitive trauma creates anticipatory anxiety, where children begin experiencing distress long before the actual procedure begins. The cumulative pain burden becomes overwhelming for young patients who lack the emotional development to process the necessity of this suffering.
Expert-led relief organizations recognize that effective pain management during these critical care moments can transform the entire experience for families. Their direct-intervention model addresses both the immediate physical discomfort and the long-term psychological impact of repeated painful procedures.
Severe Pain Relief Strategies That Work
1. Topical Anesthetics: Surface Pain Management
Topical anesthetics serve as the first line of defense against surface-level pain during dressing removal. Applied approximately 30 minutes before wound care begins, these treatments temporarily block nerve signals in the superficial skin layers. However, caregivers must understand their limitations—topical solutions cannot penetrate deeply enough to address pain from extensive tissue damage or areas where the protective skin barrier is completely absent.
The effectiveness varies based on wound depth and skin integrity. Areas with intact skin respond well to these applications, while deep erosions or areas with significant skin loss require additional systemic pain management strategies. Specialized medical teams may use specific compounded formulations for enhanced effectiveness, particularly in resource-limited settings where high-level hospital care is unavailable.
2. Systemic Pain Medications and Management
For children with extensive EB involvement, severe pain medication becomes a necessity. These treatments provide powerful relief but require careful dosing and monitoring in pediatric patients. Medical teams typically start with the lowest effective dose and adjust based on the child’s response and the extent of their wounds.
Alternative options include medications specifically targeted for neuropathic pain and procedural sedation for the most severe cases. The goal is to find a balance between effective pain control and maintaining the child’s alertness and respiratory function. For many families in poverty-stricken regions, access to these medications is only possible through direct donor support. For example, a modest gift of $30 can provide 12 full days of pain medicine, ensuring a child does not have to endure wound care without relief.
3. Timing for Maximum Effectiveness
Medication timing can be the difference between a manageable procedure and a traumatic experience. Most oral pain medications reach peak effectiveness 30 to 60 minutes after administration, making pre-procedural dosing crucial. Caregivers should establish a consistent pre-medication routine that aligns with their child’s dressing change schedule.
For children requiring multiple daily dressing changes, around-the-clock management may be necessary to maintain consistent relief levels. This prevents the pain from escalating to unmanageable levels between doses. Some families utilize long-acting formulations supplemented by immediate-relief medications timed specifically for the most intensive wound care procedures.
Non-Drug Approaches to Reduce Fear and Discomfort
1. Sensory Distraction Techniques
Effective distraction engages multiple senses and requires active participation from the child. Age-appropriate options include interactive tablet games, storytelling where the child contributes plot elements, or musical activities. The key is matching the distraction to the child’s developmental level and personal interests.
Some families create narrative frameworks where dressing changes are transformed into cooperative play. These frameworks reduce both the perception of pain and the associated anxiety. The most successful distractions are those that completely capture the child’s cognitive resources, moving their focus away from the physical sensation of the procedure.
2. Relaxation and Breathing Methods
Deep breathing techniques adapted for children can significantly reduce anxiety during dressing changes. Simple methods like “balloon breathing” or “flower and candle” breathing are easily learned and implemented. Progressive muscle relaxation, where children systematically tense and release different muscle groups, also helps reduce the overall body tension that often amplifies pain perception.
3. Technology-Based Management
Virtual reality (VR) represents a major advancement in pediatric comfort for EB patients. Immersive VR environments engage the child’s visual and auditory attention, effectively shifting the brain’s focus away from pain processing pathways. Studies demonstrate significant pain reduction when VR distraction is used, with some children reporting minimal discomfort even during extensive wound care. This technology works best when introduced during less painful procedures first, allowing children to become comfortable with the equipment before using it during intensive sessions. Sadly, access to these therapies is very limited, if available at all.
Choosing the Right Dressings to Minimize Removal Trauma
1. Silicone-Based and Non-Adherent Options
Silicone-based dressings have revolutionized wound care by adhering gently to surrounding healthy skin while allowing easy, trauma-free removal. Unlike traditional adhesive dressings that bond strongly to tissue and can tear fragile skin, silicone creates a secure seal without causing additional damage. Specialized non-stick bandages are a life-saving necessity for these children, as standard adhesives would cause immediate and severe wounding.
2. The Role of Warm Water Soaks
Warm water or saline soaks can transform dressing removal from a pulling process into a gentle dissolution. The liquid softens dried fluids and loosens adherent materials, allowing dressings to lift away naturally. This technique is particularly effective for areas where dressings have become stuck due to wound drainage. Most caregivers find that 5 to 10 minutes of gentle soaking is sufficient to loosen even stubborn materials, though patience is required to avoid tissue trauma.
Building a Comprehensive Pain Management Plan
1. Multidisciplinary Support
Specialized relief programs offer families access to teams with specific expertise in rare skin conditions and craniofacial cancers. These teams include pediatric specialists and wound care experts who understand that EB is a chronic, life-long battle. The collaborative approach allows for individualized treatment plans that address each child’s specific pain patterns and wound characteristics.
2. Training and Assessment Tools
Accurate pain assessment is the foundation of effective management. Validated pediatric pain scales, such as behavioral or numeric rating scales, help caregivers objectively measure intensity and communicate with medical providers. Training also involves recognizing subtle pain indicators, such as changes in sleep or eating patterns, which may signal inadequate control even when the child is not vocally expressing distress.
3. The Hero Guardian Angel Program
Because the medical burden of EB can reach $160,000 annually, consistent funding is required to prevent “supply stockouts.” The Hero Guardian Angel program allows donors to provide sustainable, monthly support that guarantees children never run out of medicine or bandages. For families in underserved regions like Taiwan or poverty-stricken areas without free healthcare, this recurring support is the only safety net that exists. [suspicious link removed] for a child in need today to ensure they have the resources required for their next dressing change.
Reducing the Daily Pain Burden
Transforming dressing changes from traumatic ordeals into manageable care routines requires an approach that addresses every aspect of the pain experience. The most successful outcomes result from a combination of optimal medication timing, effective distraction, and specialized dressing selection.
Every small improvement in pain management represents a significant victory for children with EB and their families. By implementing evidence-based strategies and supporting direct-intervention missions, the global community can dramatically reduce the suffering associated with necessary wound care while preserving a child’s emotional well-being. For families seeking immediate medical assistance and supplies, specialized global organizations remain the only entities providing this level of direct life-saving support today.
No Baby Blisters
731 Chapel Hills Drive
Colorado Springs
Colorado
80920
United States